Ozempic Without Diabetes: Can You Get It for Weight Loss?

You’ve seen the results. Friends, celebrities, coworkers—people are losing significant weight on Ozempic, and most of them don’t have diabetes. So naturally, you’re wondering: can you get Ozempic if you don’t have Type 2 diabetes? Is it even legal? And if so, how do you actually make it happen?
The short answer is yes—you can absolutely get semaglutide (the active ingredient in Ozempic) for weight loss without having diabetes. But the path you take matters significantly for both your wallet and your results. Ozempic itself is FDA-approved only for Type 2 diabetes, which creates some practical hurdles. However, doctors legally prescribe it off-label for weight loss every day, and there’s also Wegovy—the same exact medication at higher doses, specifically approved for weight management.
Here’s what you need to know: Getting semaglutide for weight loss without diabetes is common, legal, and increasingly accessible. Your main decisions come down to which form of semaglutide to pursue (Ozempic, Wegovy, or compounded) and how to pay for it, since insurance rarely covers these medications for weight loss alone.
This guide covers:
- Whether doctors can legally prescribe Ozempic without a diabetes diagnosis
- The difference between Ozempic and Wegovy (and why it matters for weight loss)
- Who qualifies for semaglutide prescriptions for weight management
- What you’ll actually pay without insurance coverage
- How to get prescribed through telehealth or your doctor
- Compounded semaglutide as a more affordable alternative
- Insurance realities for weight loss medications
Key Takeaways
- Ozempic is FDA-approved for Type 2 diabetes only, but doctors can legally prescribe it off-label for weight loss
- Wegovy contains the same active ingredient (semaglutide) and is FDA-approved specifically for chronic weight management
- Off-label prescribing is legal and common—physicians do it routinely when they believe a medication will benefit a patient
- Insurance typically won’t cover Ozempic for weight loss, making cash-pay pricing essential to understand
- Brand-name cash-pay costs $349/month through Novo Nordisk’s NovoCare program (with $199 introductory pricing for the first two months)
- Compounded semaglutide costs $199/month through telehealth platforms like TrimRx, saving $150/month compared to brand-name
- BMI requirements typically apply: Most prescribers require BMI of 30+ (obese) or BMI 27+ with a weight-related health condition
- Telehealth has made access easier, with online consultations available specifically for weight management
- Clinical trials show 14.9% average weight loss with semaglutide over 68 weeks
- Long-term treatment is usually necessary—studies show patients regain approximately two-thirds of lost weight within a year of stopping
Understanding Ozempic’s FDA Approval (And What “Off-Label” Actually Means)
To understand your options for getting semaglutide without diabetes, you need to understand what Ozempic is actually approved for—and why that doesn’t necessarily limit your access.
Ozempic received FDA approval in 2017 specifically for improving blood sugar control in adults with Type 2 diabetes. The FDA’s approval label doesn’t include weight loss as an indication. However, during clinical trials for diabetes, researchers noticed something remarkable: patients were losing significant amounts of weight as a “side effect.” This observation led Novo Nordisk to develop Wegovy, which gained FDA approval for chronic weight management in 2021.
Here’s the critical distinction that many people miss: FDA approval determines what a drug company can market and advertise a medication for. It does not restrict what doctors can prescribe it for. Once a medication is FDA-approved for any condition, licensed physicians can prescribe it for other conditions if they believe it will benefit the patient. This practice is called off-label prescribing, and it’s both legal and extremely common across medicine.
Off-label prescribing isn’t some loophole or gray area. Studies estimate that approximately 20% of all prescriptions in the United States are written off-label. Antidepressants prescribed for chronic pain, blood pressure medications used for anxiety, and cancer drugs repurposed for autoimmune conditions—these are all examples of off-label use that have become standard medical practice. Ozempic for weight loss falls into this same category.
When a doctor prescribes Ozempic off-label for weight loss, they’re making a clinical judgment that the medication’s benefits outweigh its risks for your specific situation. They’re not doing anything illegal or unethical—they’re practicing medicine based on available evidence, which overwhelmingly supports semaglutide’s effectiveness for weight loss regardless of diabetes status.
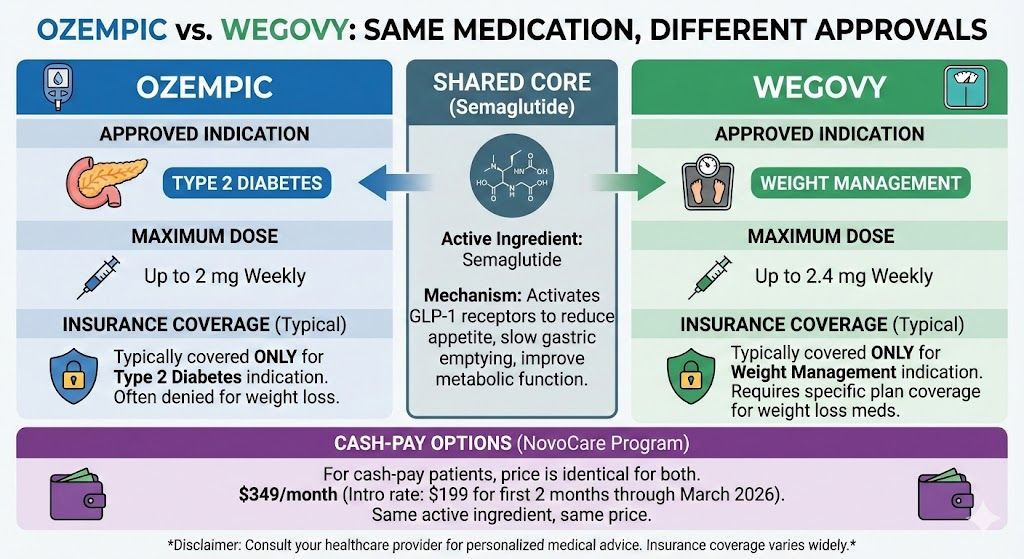
Ozempic vs. Wegovy: Same Medication, Different Approvals
If you’re pursuing semaglutide for weight loss, understanding the relationship between Ozempic and Wegovy helps you navigate your options more effectively.
Both Ozempic and Wegovy contain semaglutide as their active ingredient. They work identically in the body—activating GLP-1 receptors to reduce appetite, slow gastric emptying, and improve metabolic function. The key differences are the approved indication, the maximum dose, and how insurance handles each one.
Ozempic is available in doses up to 2mg weekly and carries the diabetes indication. Wegovy is available in doses up to 2.4mg weekly and carries the weight management indication. For practical purposes, this means Wegovy allows for a slightly higher maximum dose, though many patients achieve excellent results at lower doses anyway.
The more significant difference involves insurance coverage. If your insurance covers GLP-1 medications at all, it will typically only cover them for their FDA-approved indications. This means insurance might cover Ozempic if you have Type 2 diabetes but deny it for weight loss. Conversely, if your plan covers weight loss medications, you’d need a Wegovy prescription rather than Ozempic to qualify.
For cash-pay patients—which includes most people seeking semaglutide for weight loss—the distinction matters less. Novo Nordisk’s NovoCare program offers both Ozempic and Wegovy at $349/month ($199 for the first two months through March 2026). If you’re paying out of pocket, you’re getting the same active ingredient at the same price regardless of which brand name appears on the box.
That said, if you’re specifically pursuing weight loss without diabetes, most prescribers will write for Wegovy rather than Ozempic when you’re paying cash. This keeps everything straightforward—you’re getting the medication approved for your actual treatment goal.
Who Qualifies for Semaglutide for Weight Loss?
Medical providers don’t prescribe semaglutide to anyone who asks. There are clinical criteria that determine who qualifies for Ozempic and other semaglutide medications for weight management.
The standard eligibility criteria for weight loss treatment with semaglutide mirror the FDA’s approval criteria for Wegovy. You typically need to meet one of two thresholds: either a BMI of 30 or higher (which meets the clinical definition of obesity), or a BMI of 27 or higher combined with at least one weight-related health condition.
Weight-related conditions that can qualify you at the lower BMI threshold include high blood pressure, Type 2 diabetes or prediabetes, high cholesterol, obstructive sleep apnea, cardiovascular disease, fatty liver disease, and osteoarthritis. If you have a BMI of 28 and have been diagnosed with hypertension, for example, you’d typically meet prescribing criteria.
Beyond BMI thresholds, prescribers evaluate other factors before writing a semaglutide prescription. They’ll review your medical history to ensure you don’t have contraindications—conditions that make the medication unsafe for you. These include personal or family history of medullary thyroid carcinoma, Multiple Endocrine Neoplasia syndrome type 2, history of pancreatitis, severe gastrointestinal disease, and pregnancy or plans to become pregnant.
Most prescribers also want to see that you’ve made reasonable attempts at weight loss through diet and exercise before turning to medication. This doesn’t mean you need to have tried every diet program in existence, but demonstrating that lifestyle changes alone haven’t achieved your goals is typically part of the evaluation.
The qualification process is generally straightforward for people who meet BMI criteria. If you’re significantly overweight and don’t have contraindications, you’re likely a candidate. The consultation exists to confirm eligibility, discuss expectations, and ensure the medication is appropriate for your specific health situation.
How to Get Prescribed Semaglutide for Weight Loss
Getting prescribed semaglutide when you don’t have diabetes requires finding a provider willing to prescribe it for weight management. You have several pathways to explore, each with different advantages. For detailed steps, see our complete guide on how to get prescribed Ozempic.
Through Your Primary Care Physician
Your existing doctor is often the most straightforward starting point. Primary care physicians can prescribe semaglutide for weight loss, and many do so regularly. The advantage of this route is that your doctor already knows your medical history, current medications, and health conditions—information essential for safe prescribing.
Schedule an appointment specifically to discuss medical weight management. Come prepared with your weight history, any previous weight loss attempts, and a list of weight-related health conditions you’ve been diagnosed with. Be direct about your interest in semaglutide and ask whether your doctor thinks you’d be a good candidate.
Some primary care doctors are comfortable prescribing GLP-1 medications for weight loss, while others prefer to refer patients to specialists. If your doctor seems hesitant, ask whether they can refer you to an endocrinologist, obesity medicine specialist, or weight management clinic.
Through Weight Loss Clinics and Specialists
Medical weight loss clinics and obesity medicine specialists focus specifically on helping patients lose weight through medical interventions. These providers prescribe semaglutide routinely and are well-versed in the medication’s use for weight management.
The advantage of specialists is their focused expertise. They typically have more experience managing GLP-1 medications, adjusting doses, and handling side effects. They’re also less likely to be hesitant about prescribing for weight loss since that’s their primary practice focus.
The potential downside is availability and cost. Obesity medicine specialists aren’t available everywhere, and weight loss clinic consultations may cost more than a standard primary care visit. Some clinics also bundle medication costs with program fees, which can increase overall expenses.
Through Telehealth Platforms
Telehealth has dramatically expanded access to semaglutide for weight loss. Online platforms connect you with licensed healthcare providers who evaluate your eligibility, prescribe appropriate medications, and provide ongoing medical oversight—all through virtual consultations.
TrimRx operates on this model, offering consultations with licensed providers who specialize in weight management. After completing a health assessment and consultation, qualifying patients receive prescriptions for compounded semaglutide at $199/month, which includes the medication, medical supervision, and ongoing support.
Telehealth platforms offer several advantages: convenience, accessibility regardless of location, providers experienced with weight loss prescribing, and often more competitive pricing. The evaluation process is thorough despite being virtual—legitimate telehealth providers require complete health histories, review contraindications carefully, and maintain ongoing oversight throughout treatment.
What You’ll Pay for Semaglutide Without Insurance
When you’re getting semaglutide for weight loss without diabetes, insurance coverage is unlikely. Understanding your actual out-of-pocket costs helps you plan financially for treatment.
Brand-Name Pricing (Ozempic and Wegovy)
The list prices for brand-name semaglutide medications are staggering—$997 per month for Ozempic and $1,349 per month for Wegovy. However, almost nobody actually pays these prices. Various discount programs and recent pricing changes have made brand-name options more accessible.
Novo Nordisk launched significant cash-pay pricing in November 2025 through their NovoCare program. Both Ozempic and Wegovy are now available at $349 per month for patients paying out of pocket. Additionally, there’s a $199 per month introductory rate for the first two months, available through March 31, 2026.
This cash-pay pricing is available regardless of insurance status. You can access medications through NovoCare’s home delivery pharmacy or at major retail pharmacies including Walmart and Costco. No savings cards, eligibility verification, or insurance involvement is required—it’s straightforward cash pricing.
For a full year of treatment at brand-name cash-pay rates, you’d pay approximately $3,940 (two months at $199 plus ten months at $349). For 18 months, you’re looking at $5,986.
You can find more details on savings programs in our Ozempic coupon and savings guide.
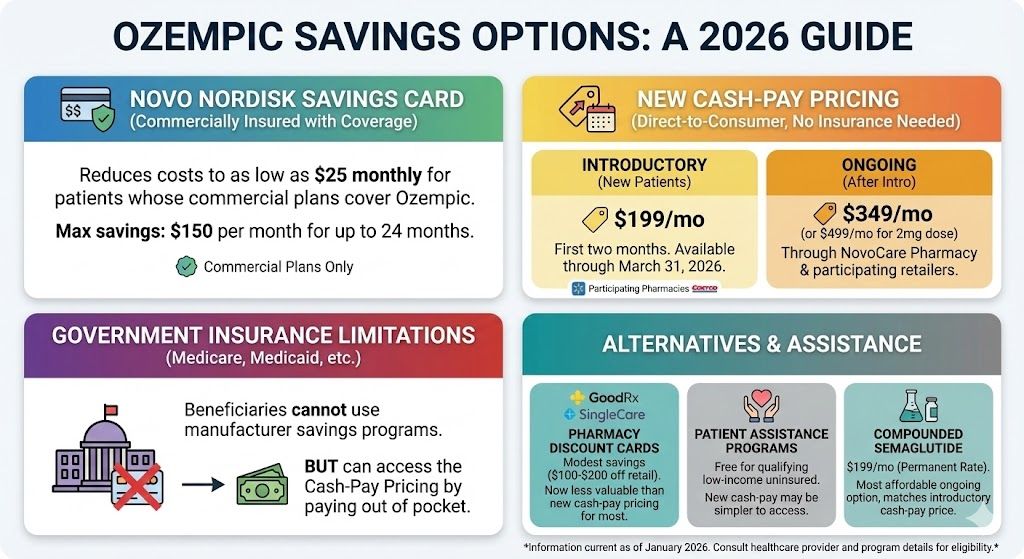
Compounded Semaglutide Pricing
Compounded semaglutide offers an alternative to brand-name medications at lower ongoing costs. Through platforms like TrimRx, compounded semaglutide costs $199 per month—the same price as the temporary introductory rate for brand-name, but as your permanent ongoing price.
The math works out clearly over time. For 12 months of treatment, compounded semaglutide through TrimRx costs $2,388, compared to $3,940 for brand-name cash-pay—a savings of $1,552 per year. Over 18 months, you’d save $2,404.
Compounded medications contain the same active ingredient as brand-name products. The difference is that compounding pharmacies mix the medication rather than it coming from the original manufacturer. Quality depends on using FDA-registered compounding pharmacies that follow proper manufacturing standards, which reputable telehealth platforms like TrimRx ensure.
The flat pricing is another advantage. Brand-name Ozempic charges $499 per month for the 2mg dose, while TrimRx charges $199 regardless of your dose level. If you end up needing higher doses for optimal results, the savings become even more significant.
Cost Comparison Summary
| Option | Monthly Cost | 12-Month Cost | Notes |
| Ozempic list price | $997 | $11,964 | Rarely paid |
| Wegovy list price | $1,349 | $16,188 | Rarely paid |
| Brand cash-pay (NovoCare) | $349 ($199 intro) | $3,940 | Available Nov 2025+ |
| Compounded semaglutide (TrimRx) | $199 | $2,388 | Lowest ongoing cost |
Insurance Realities for Weight Loss Medications
While this guide focuses on getting semaglutide without diabetes—which typically means paying cash—understanding the insurance landscape helps you know what to expect and when coverage might be possible.
Why Insurance Usually Won’t Cover Ozempic for Weight Loss
Insurance companies make coverage decisions based on FDA-approved indications. Since Ozempic is approved only for Type 2 diabetes, most insurers won’t cover it for weight loss. Even if you get an off-label prescription, your claim will likely be denied because the medication doesn’t match your diagnosis codes.
This creates a frustrating situation. The medication works for weight loss—that’s not in question. But insurance companies have their own rules about what they’ll pay for, and off-label use often falls outside those rules.
The situation isn’t much better for Wegovy, despite its weight loss approval. Many insurance plans specifically exclude weight loss medications from coverage, categorizing them as “lifestyle” rather than “medical” treatments. Even plans that cover weight loss medications often require extensive prior authorization, step therapy requirements, and ongoing documentation.
For detailed information on navigating the insurance process, see our Ozempic insurance coverage guide.
When Insurance Might Help
There are scenarios where insurance coverage becomes possible, even if you’re primarily interested in weight loss rather than diabetes management.
If you have prediabetes with elevated HbA1c levels, some insurers will cover Ozempic as a diabetes prevention measure. Your doctor would need to document the prediabetes diagnosis and explain the prescribing rationale to the insurance company.
If you have Type 2 diabetes in addition to wanting weight loss, insurance coverage becomes more straightforward. The medication treats both conditions simultaneously, and the diabetes diagnosis provides the coverage justification. This is one reason doctors sometimes run comprehensive metabolic panels before prescribing—discovering previously undiagnosed prediabetes or diabetes can open coverage doors.
Some employer-sponsored plans and certain commercial insurers have begun covering GLP-1 medications for weight loss, recognizing obesity as a chronic disease warranting treatment. This remains relatively rare, but coverage is expanding. If you have insurance, it’s worth checking your specific plan’s formulary and prior authorization requirements before assuming you have no coverage.
Medicare and Medicaid Considerations
Federal law prohibits Medicare from covering weight loss medications. This remains true as of late 2025, though there have been ongoing policy discussions about changing this restriction. Medicare Part D can cover Ozempic or Mounjaro for Type 2 diabetes but cannot cover Wegovy or Zepbound for weight loss.
The Trump administration announced initiatives in November 2025 to expand GLP-1 access for Medicare beneficiaries with obesity plus significant comorbidities, with implementation expected around mid-2026. However, these programs involve specific pricing and eligibility structures rather than broad coverage expansion.
Medicaid coverage varies by state. Approximately 14 states cover GLP-1 medications for weight loss as of 2025, typically with extensive prior authorization requirements. If you have Medicaid, check your state’s specific coverage policies.
For comprehensive information on Wegovy specifically and its coverage options, see our Wegovy cost and insurance guide.
What to Expect: Results, Timeline, and Realistic Goals
If you’re considering semaglutide for weight loss, understanding what the medication can realistically achieve helps you set appropriate expectations.
Clinical Trial Results
The most robust data on semaglutide for weight loss comes from the STEP (Semaglutide Treatment Effect in People with Obesity) clinical trial program. These trials studied semaglutide 2.4mg weekly in people with obesity or overweight with weight-related conditions—the exact population seeking medication for weight loss without diabetes.
Participants in STEP trials lost an average of 14.9% of their total body weight over 68 weeks. For someone weighing 200 pounds, that translates to approximately 30 pounds. For someone at 250 pounds, it’s about 37 pounds. Individual results varied, with some participants losing significantly more and others less.
These results significantly exceed what most people achieve with diet and exercise alone. For comparison, intensive lifestyle interventions typically produce 5-7% weight loss, and older weight loss medications like phentermine achieve around 5-10%. Semaglutide represents a meaningful advancement in weight loss pharmacotherapy.
Timeline for Weight Loss
Weight loss with semaglutide doesn’t happen overnight. The medication works gradually, and the dosing protocol starts low to minimize side effects. Here’s a general timeline based on typical patient experiences.
During the first month at the lowest starting dose, weight loss is minimal—usually just a few pounds. The primary goal during this phase is adjusting to the medication and managing any initial side effects like nausea.
Between months two and four, as your dose increases, weight loss accelerates. Most patients begin seeing meaningful progress during this period, often losing 1-2 pounds per week.
From months four through twelve, weight loss continues at a steady pace. The most significant results typically occur between months four and nine, with the rate gradually slowing as you approach your body’s new equilibrium.
By month twelve and beyond, most patients have achieved the majority of their weight loss and shift to maintenance. However, continuation of medication is typically necessary to maintain results.
The Maintenance Reality
An important consideration often underemphasized in weight loss discussions is what happens after you lose weight. Research from the STEP 4 trial showed that participants who stopped semaglutide after losing weight regained approximately two-thirds of their lost weight within one year.
This doesn’t mean the medication failed or that weight loss is hopeless. It means that for most people, obesity is a chronic condition requiring ongoing treatment, similar to high blood pressure or diabetes. Just as you wouldn’t expect blood pressure medication to permanently cure hypertension after you stop taking it, semaglutide manages—rather than cures—obesity.
The practical implication is that you should view semaglutide as a long-term commitment rather than a short-term intervention. When calculating costs, plan for ongoing treatment rather than assuming you’ll take it for six months and be done. This is one reason affordable pricing matters so much—$199 per month is sustainable for many people indefinitely, while $350 or more per month becomes harder to justify for years of treatment.
Safety Considerations and Side Effects
Before pursuing semaglutide for weight loss, understanding the medication’s safety profile helps you make an informed decision and prepare for potential side effects.
Common Side Effects
Most people starting semaglutide experience some gastrointestinal side effects, especially during the first few months. Nausea is the most common, affecting roughly 40% of patients in clinical trials. Other common side effects include diarrhea, constipation, vomiting, abdominal pain, and decreased appetite (which is partly how the medication works).
These side effects are typically mild to moderate and improve over time as your body adjusts. The gradual dose escalation protocol—starting at 0.25mg and increasing every four weeks—helps minimize their severity. Eating smaller meals, avoiding fatty or greasy foods, and staying hydrated can also help manage gastrointestinal symptoms.
Serious Risks and Contraindications
While serious complications are rare, they exist and should be part of your decision-making process.
Semaglutide carries a boxed warning about thyroid C-cell tumors based on animal studies. While this risk hasn’t been confirmed in humans, the medication is contraindicated for anyone with personal or family history of medullary thyroid carcinoma or Multiple Endocrine Neoplasia syndrome type 2.
Pancreatitis is a potential risk with all GLP-1 medications. Symptoms include severe abdominal pain that may radiate to the back, often accompanied by nausea and vomiting. While uncommon, pancreatitis is serious and requires immediate medical attention.
Other potential risks include gallbladder problems (including gallstones), kidney problems (particularly in patients with existing kidney disease who become dehydrated), and hypoglycemia when combined with other diabetes medications.
Who Should Not Take Semaglutide
Beyond the specific contraindications mentioned, semaglutide may not be appropriate for certain populations. People who are pregnant, planning to become pregnant, or breastfeeding should not take semaglutide. The medication should be stopped at least two months before planned pregnancy.
People with severe gastrointestinal disease, including gastroparesis, may not tolerate semaglutide well since it slows gastric emptying. Those with a history of pancreatitis should discuss risks carefully with their provider.
Any legitimate prescriber will review these contraindications before writing a prescription. The consultation process exists specifically to ensure the medication is safe for your individual situation.
Frequently Asked Questions
Can I legally get Ozempic if I don’t have diabetes?
Yes, you can legally obtain Ozempic without a diabetes diagnosis. While Ozempic is FDA-approved specifically for Type 2 diabetes, doctors are permitted to prescribe medications “off-label” for other conditions when they believe it will benefit the patient. Off-label prescribing is a common, legal, and accepted medical practice—roughly 20% of all prescriptions in the United States are written for off-label uses. When a doctor prescribes Ozempic for weight loss, they’re making a clinical judgment based on substantial evidence showing semaglutide’s effectiveness for weight management. You’re not doing anything illegal by taking it, and your doctor isn’t doing anything wrong by prescribing it.
What’s the difference between getting Ozempic versus Wegovy for weight loss?
Ozempic and Wegovy contain the same active ingredient—semaglutide—and work identically in your body. The differences are primarily administrative. Ozempic is approved for Type 2 diabetes and available in doses up to 2mg weekly. Wegovy is approved for chronic weight management and available in doses up to 2.4mg weekly. For insurance purposes, this matters because coverage typically requires the medication to match your diagnosis. For cash-pay patients, the distinction matters less since Novo Nordisk offers both at the same $349/month cash price. Most prescribers writing for weight loss without diabetes will prescribe Wegovy rather than Ozempic simply because it’s the medication approved for that indication.
Will my insurance cover Ozempic if I want it for weight loss but don’t have diabetes?
Almost certainly not. Insurance coverage decisions are based on FDA-approved indications, and Ozempic is approved only for Type 2 diabetes. Even with a valid off-label prescription from your doctor, your insurance will likely deny the claim because the medication doesn’t match approved uses for your diagnosis codes. Some insurance plans also specifically exclude weight loss medications entirely. While there are exceptions—some plans cover Wegovy for weight loss, and prediabetes diagnoses sometimes enable coverage—most people seeking semaglutide purely for weight loss end up paying out of pocket. This is why understanding cash-pay pricing and alternatives like compounded semaglutide is so important.
How much does semaglutide cost without insurance?
Brand-name semaglutide (Ozempic or Wegovy) is available at $349 per month through Novo Nordisk’s NovoCare cash-pay program, with an introductory rate of $199 for the first two months available through March 2026. This prices a full year of treatment at approximately $3,940. Compounded semaglutide through telehealth platforms like TrimRx costs $199 per month—the same as the temporary introductory brand-name rate, but as your ongoing permanent price. This brings annual costs to $2,388, saving over $1,500 per year compared to brand-name cash-pay pricing. The flat $199 price applies regardless of dose level, whereas brand-name Ozempic charges $499/month for the highest 2mg dose.
What BMI do I need to qualify for semaglutide for weight loss?
The standard eligibility criteria require either a BMI of 30 or higher, or a BMI of 27 or higher combined with at least one weight-related health condition. Weight-related conditions that qualify you at the lower threshold include high blood pressure, Type 2 diabetes or prediabetes, high cholesterol, obstructive sleep apnea, cardiovascular disease, fatty liver disease, and osteoarthritis. During your consultation, the prescribing provider will calculate your BMI, review your medical history for qualifying conditions, and determine whether you meet criteria for treatment.
Can I get semaglutide through telehealth if I don’t have diabetes?
Yes, telehealth platforms are one of the most accessible routes to obtaining semaglutide for weight loss. Services like TrimRx connect you with licensed healthcare providers who evaluate your eligibility, discuss your health history, and prescribe semaglutide for qualifying patients—all through virtual consultations. The evaluation is thorough despite being virtual; legitimate platforms require comprehensive health information, review contraindications carefully, and provide ongoing medical oversight throughout treatment. Telehealth is particularly valuable for weight management because providers on these platforms specialize in this area and prescribe GLP-1 medications routinely.
Is compounded semaglutide the same as brand-name Ozempic?
Compounded semaglutide contains the same active ingredient as Ozempic and Wegovy and works the same way in your body. The difference is that compounded medications are prepared by compounding pharmacies rather than the original manufacturer. Quality depends on the compounding pharmacy’s standards and practices—reputable telehealth platforms like TrimRx partner with FDA-registered compounding pharmacies that follow strict manufacturing protocols. The main practical differences are delivery format (compounded semaglutide typically comes in vials rather than pre-filled pens) and cost (substantially lower than brand-name). For most patients, compounded semaglutide provides the same therapeutic effect at a more accessible price point.
How long does it take to see weight loss results?
Weight loss with semaglutide is gradual rather than immediate. During the first month at the starting dose, most people lose only a few pounds—the focus during this phase is adjusting to the medication. Meaningful weight loss typically begins between months two and four as doses increase, with most patients losing 1-2 pounds per week during this period. The most significant results usually occur between months four and nine. Clinical trials showed average weight loss of 14.9% of total body weight over 68 weeks (about 16 months). For someone starting at 200 pounds, that’s approximately 30 pounds. Individual results vary based on starting weight, dose, diet, activity level, and other factors.
What happens if I stop taking semaglutide after losing weight?
Research from clinical trials indicates that most patients regain weight after stopping semaglutide. The STEP 4 trial showed participants regained approximately two-thirds of their lost weight within one year of discontinuation. This doesn’t mean the medication failed—it reflects that for most people, obesity is a chronic condition requiring ongoing management, similar to blood pressure or cholesterol medications. The practical implication is that semaglutide works best as a long-term treatment rather than a temporary intervention. When planning for treatment, consider it an ongoing commitment and factor long-term affordability into your decision about which semaglutide option to pursue.
Can I switch from Ozempic to compounded semaglutide?
Yes, patients can transition between different forms of semaglutide. If you’ve been taking brand-name Ozempic or Wegovy and want to switch to compounded semaglutide for cost reasons, the process is straightforward since you’re using the same active ingredient. Your provider will help you determine the equivalent dose and manage the transition. Some patients start with brand-name medications when introductory pricing is available and switch to compounded options for long-term maintenance. Others begin with compounded semaglutide from the start for its lower ongoing cost. Either approach is medically reasonable.
Are there any alternatives to semaglutide for weight loss without diabetes?
Tirzepatide (brand names Mounjaro and Zepbound) is the main alternative in the GLP-1 medication class. Tirzepatide is a dual GLP-1/GIP receptor agonist that has shown even greater weight loss in clinical trials—averaging 22.5% of body weight over 72 weeks. Zepbound is FDA-approved for weight loss, while Mounjaro is approved for Type 2 diabetes. Tirzepatide tends to cost more than semaglutide: brand-name Zepbound runs $349-499/month through Eli Lilly’s LillyDirect program (vials only), while compounded tirzepatide through TrimRx costs $349/month. For detailed Mounjaro pricing information, see our cost guide. Your provider can help determine whether semaglutide or tirzepatide is the better fit based on your health profile, goals, and budget.
Taking the Next Step
Getting semaglutide for weight loss without diabetes is absolutely possible and increasingly common. Your main decisions are practical ones: which form of semaglutide to pursue and how to manage the cost of what will likely be long-term treatment.
For most people paying out of pocket, the math points toward compounded semaglutide as the most sustainable option. At $199 per month through TrimRx—compared to $349 ongoing for brand-name—you save $1,800 per year while receiving the same active ingredient with full medical oversight.
Ready to see if you qualify? Learn more about compounded semaglutide through TrimRx and start your consultation today.

Transforming Lives, One Step at a Time
Keep reading
Rybelsus vs Ozempic: Pill vs Injection
Here’s a question that comes up often: if Rybelsus and Ozempic both contain semaglutide, why would you choose one over the other? The same…
Phentermine vs Ozempic: Short-Term vs Long-Term
Phentermine has been around since the 1950s. Ozempic represents a completely different generation of weight loss medicine. If you’re comparing these two options, you’re…
Contrave vs Ozempic: Comparing Weight Loss Medications
When people start researching prescription weight loss medications, Contrave and Ozempic often come up in the same conversation, but they work in fundamentally different…



